When most people hear the word estrogen, they think of periods, fertility, or menopause. Occasionally they think of PMS. Rarely do they think of mood regulation, cognition, stress tolerance, or emotional resilience due to the limited conversations we have in life about female hormones. This educational gap is problem, because estrogen is deeply involved in all of them.
Before getting into mental health more broadly, let’s zoom out and correct the framing.
A few estrogen facts that rarely make it into mental health conversations:
- Estrogen directly influences serotonin, dopamine, and norepinephrine — the same neurotransmitters targeted by many psychiatric medications (Bethea et al., 2002; Borrow & Cameron, 2014)
- Estrogen modulates brain-derived neurotrophic factor (BDNF), which supports learning, neuroplasticity, and emotional regulation (Scharfman & MacLusky, 2006)
- Estrogen is neuroprotective, supporting cerebral blood flow, glucose metabolism, and anti-inflammatory processes in the brain (Brinton, 2009)
- Estrogen receptors are widely distributed throughout the brain — including the hippocampus, amygdala, and prefrontal cortex (McEwen & Milner, 2017)
- Fluctuations in estrogen can alter stress sensitivity and emotional processing (Albert et al., 2015)
Fun fact: estrogen also plays a protective role in vascular and cardiovascular health (Mendelsohn & Karas, 2005). This is the reason that the leading cause of death for post menopausal women is heart disease. That matters for mental health because the brain is highly dependent on stable blood flow and metabolic regulation. Mental health does not operate separately from circulation or inflammation.
Estrogen is not just a reproductive hormone. It’s a systemic pillar for overall.
Why Estrogen Matters for Mood
Mental health conversations often center on cognition, trauma history, or attachment patterns. Those factors do matter, but they are effected by our biological environment.
Estrogen helps regulate:
- Emotional reactivity
- Stress recovery
- Sensitivity to perceived threat
- Motivation and reward circuitry
- Cognitive flexibility
Research consistently shows that periods of rapid estrogen fluctuation — such as the late luteal phase, postpartum, and perimenopause — are associated with increased risk for anxiety and depressive symptoms in vulnerable individuals (Gordon et al., 2015; Soares, 2014).
What’s important here is not that estrogen “causes” mood disorders. It’s that hormonal shifts can lower the threshold at which symptoms emerge.
When estrogen levels shift, people often report:
- Increased anxiety or irritability
- Lower mood or emotional flatness
- Reduced stress tolerance
- Brain fog or slowed cognition
- Feeling “not like themselves”
And yet, standard lab ranges may still read as normal. This is also why perimenopause can be hard to catch and as well as why menopause can feel like such an abduction of self. “Normal” levels on blood tests also reflect population averages. It does not always reflect optimal function for a specific individual.
The Estrogen–Stress Feedback Loop
Estrogen and the stress response are tightly interconnected.
Chronic stress can suppress reproductive hormone signaling via the hypothalamic–pituitary–gonadal (HPG) axis. At the same time, reduced or fluctuating estrogen can increase stress sensitivity through effects on the hypothalamic–pituitary–adrenal (HPA) axis (Young & Korszun, 2010).
This creates a feedback loop:
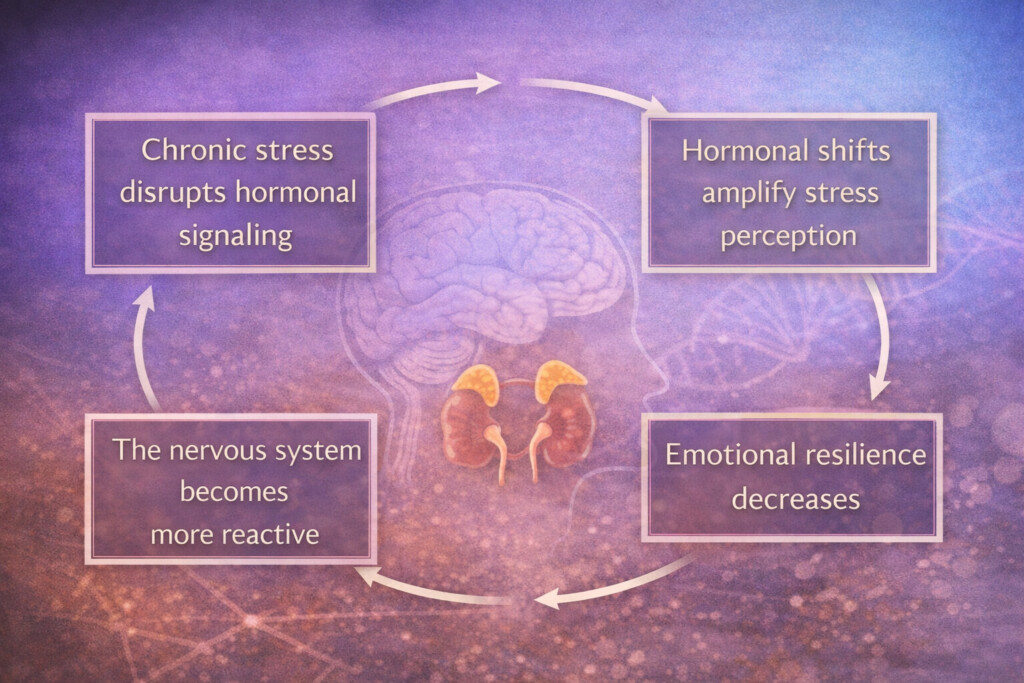
This is not because someone lacks coping skills, but because the biological terrain has shifted.
This dynamic helps explain why some individuals notice mood destabilization during:
- High cognitive or emotional load
- Under-eating or excessive exercise
- Significant life transitions
- Perimenopause/ menopause
The symptoms may look psychological. The contributing factors are often physiological.
Why Estrogen-Related Mental Health Shifts Are Often Misinterpreted
When emotional symptoms intensify, the default response is often psychiatric categorization: diagnosis, medication adjustment, behavioral strategy.
Sometimes that is necessary.
However, research suggests that estrogen-sensitive mood shifts are frequently cyclical, context-dependent, and state-based, rather than fixed personality traits (Gordon et al., 2015). Without hormone literacy, individuals may internalize these shifts as instability or fragility. Over time, this erodes self-trust.
Understanding estrogen does not replace therapy but instead refines it allowing clinicians and individuals to ask:
- Is this a persistent pattern or hormonally mediated?
- Is this trait-based or state-dependent?
- What else changed physiologically at the time symptoms intensified?
- These distinctions shape treatment decisions.
Mental Health Is Not Brain-Only
Psychology has historically separated the mind from the body in ways that are clinically convenient but biologically incomplete and honestly irresponsible. Estrogen reminds us that mental health emerges from:
- Neurotransmitter regulation
- Hormonal signaling
- Metabolic stability
- Inflammatory tone
- Psychological meaning-making
- These systems are interdependent.
When one shifts, the others adjust. Ignoring hormonal context does not make therapy stronger. It makes it less precise.
Why This Conversation Matters Earlier Than We Think
Hormone literacy often doesn’t enter the conversation until perimenopause — when symptoms are already disruptive.
But estrogen’s influence on mental health begins decades earlier.
Earlier awareness allows individuals to:
- Interpret mood changes with greater accuracy
- Reduce unnecessary self-pathologizing
- Identify stress–hormone interactions sooner
- Approach treatment with more nuance
This isn’t about blaming hormones for every emotional shift. Instead it’s about restoring context and filling in the gross educational gap we have as women and as practitioners in regards to women’s hormones. Mental health does not exist apart from the body; estrogen’s effects make that clear.
© 2026 Nassif Psychotherapy Co. All Rights Reserved.

Fantastic Article, thank you
Glad you liked it!